Chronic lymphocytic thyroiditis - Case 57. |
|
Clinical data: a 47-year-old woman requested an evaluation of a thyroid nodule discovered on an evaluation of weight gain.
Palpation: a nodule in the left lobe.
Results of blood test: euthyroidism with TSH-level 3.01 mIU/L.
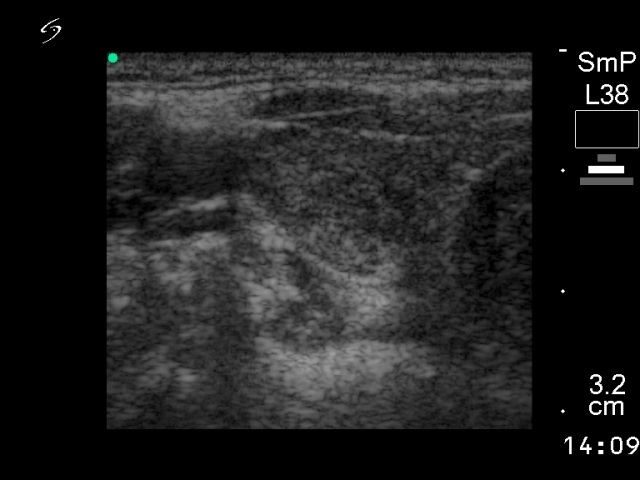
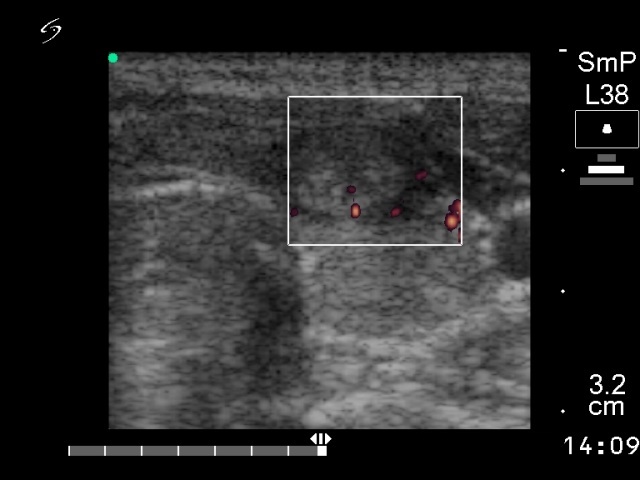
Ultrasonography: the thyroid was echonormal with small hypoechogenic foci. An echonormal nodule with a halo sign in the left lobe.
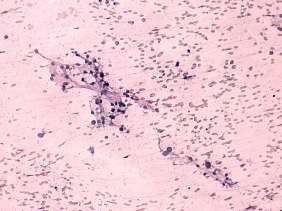
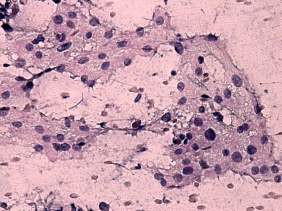
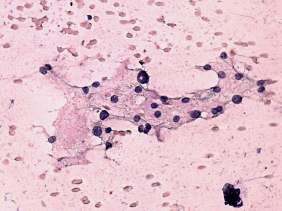
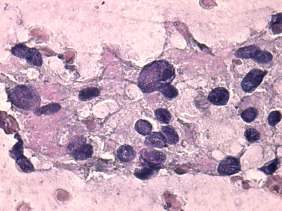
Cytological picture: no colloid in the background. Atypical, pleomorphic follicular cells in loose not specific clusters. Thyrocytes exhibit oxyphilic metaplasia.
Combined ultrasonographic-cytological diagnosis: Hürthle-cell proliferation with great probability of being benign.
Follow-up investigation: we reevaluated the patient yearly. The whole thyroid slowly became hypoechogenic, while the lesion in question disappeared in 6 years. 5 years after the original diagnosis, the patient became hypothyroid and now she is on daily 75 microgram replacement therapy. Her thyroid was atrophic, the size of the left lobe which contained the lesion, now is not greater than the original size of the lesion within the lobe 7 years earlier.
Comment: it was clear that the cytological picture alone would be suspicious for a Hürthle-cell tumor and therefore for malignancy. But there were independent factors decreasing the risk of malignancy. Firstly, the lesion was echonormal. We have found only 1 cancer among 1,898 echonormal nodules in a 8-year prospective study.
Second, the presence of small hypoechogenic foci on ultrasonography, the high-normal level of the TSH, and the oxyphilic metaplasia all independently raised the possibility that this patient had a lymphocytic thyroiditis. It seems logical, that anti-TPO determination were of help. We performed that and it resulted in a normal level (below 10 IU/mL). The problem was that in initial phase of a Hashimoto's thyroiditis, anti-TPO is rarely positive. Moreover, an elevated anti-TPO level is a proof for an autoimmune disorder, but does not exclude the possibility of malignancy.
Moreover, in a case of a well-differentiated cancer we have time to decide whether to operate a patient or not.