Papillary carcinoma - Case 40. |
|
Clinical data: a 76-year-old woman who has been operated on papillary thyroid cancer 11 years before the present examination. She underwent total thyroidectomy and irradiation. The thyroglobulin-level was below 2 ng/dl on the last visit, one year before present examination. The patient noticed a lump in the left side of the neck 2 months before present visit.
Palpation: a hard nodule left to the left carotid artery.
Functional state: subclinical hyperthyroidism on daily 125 microgram levo-tiroxin (TSH-level 0.09 mIU/L, FT4 20.8 pM/L).
Ultrasonography: there was no parenchyma according to the thyroid. Ultrasound revealed a mixed cystic-solid lesion lateral to the left thyroid bed. The solid, arborizing part of the lesion contained microcalcifications.
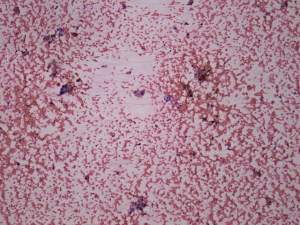
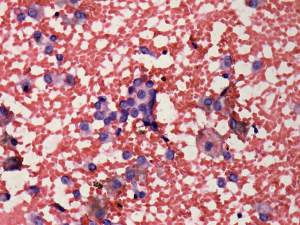
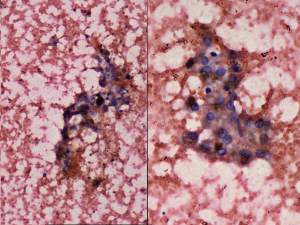
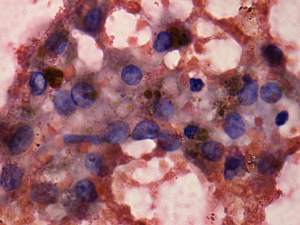
Cytological picture: small, non-specific groups of follicular cells and many macrophages were found on the smears. The degenerative changes decreased the value of the presence of nuclear inclusions.
Combined sonographic-cytological diagnosis: suspicion of papillary cancer.
Histopathology: recurrent papillary cancer.